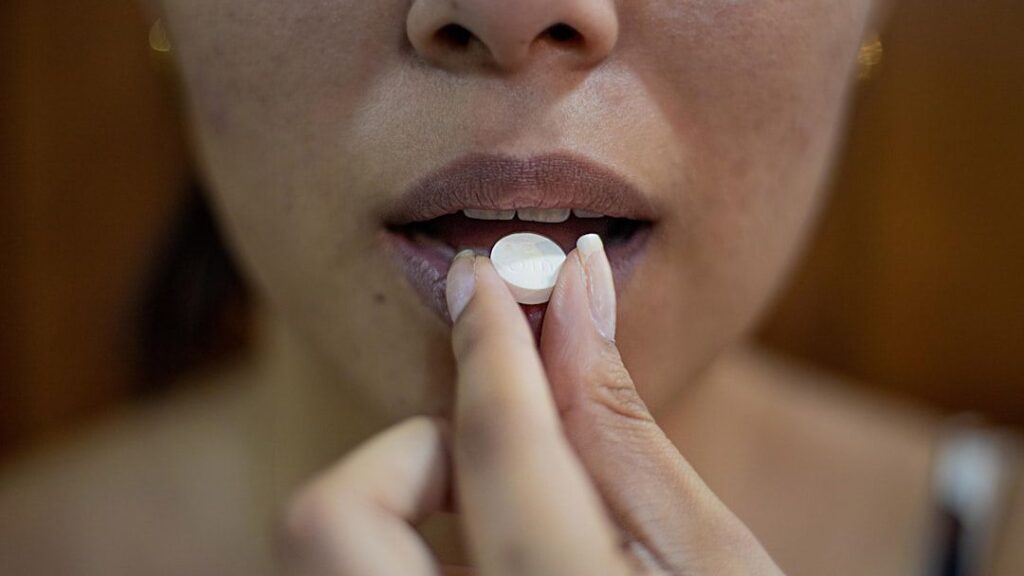
Have you ever stopped to think about the sheer power hidden inside your own head? Let’s be real, most of us tend to think healing comes from pills or procedures, and sure, those things matter. Yet there’s this bizarre, fascinating phenomenon that’s been turning medicine on its head for centuries. Your brain can convince your body that it’s healing, even when the treatment you’re receiving is nothing but a sugar pill or a fake procedure. That’s not just some philosophical mumbo jumbo, it’s backed by solid science, and honestly, it might be one of the most astonishing abilities you possess.
The placebo effect isn’t about fooling yourself or thinking positive thoughts until problems magically vanish. It goes deeper than positive thinking, creating a stronger connection between the brain and body and how they work together. Modern neuroscience has started mapping out the actual brain mechanisms at play, revealing that real physiological changes happen when you believe you’re getting better. So let’s dive in and explore just how wild this mind-body connection truly is.
Your Brain Isn’t Just Imagining Relief

When you take what you think is medicine, something remarkable happens inside your skull. Placebo treatments induce real responses in the brain, triggering neurotransmitter release, hormone production, and an immune response. It’s not like you’re pretending the pain is gone while it’s actually still there, gnawing at you. Participants who showed the most pain reduction with the placebo also showed the largest reductions in brain areas associated with pain construction. Think of it like this: your brain is actively reshaping how it processes discomfort.
Scientists have discovered that placebo responses involve increases in feel-good neurotransmitters, like endorphins and dopamine, along with greater activity in certain brain regions linked to moods, emotional reactions, and self-awareness. These aren’t vague changes that might or might not be happening. They’re measurable, they’re real, and they prove that your mind can genuinely alter your physical state. The whole thing challenges our understanding of what healing even means.
The Brain Regions That Light Up

Here’s where things get technical but stay with me because this is fascinating. Brain regions like the prefrontal cortex light up more when a patient receives a placebo treatment for pain, and this area integrates context clues like a confident doctor wearing a white coat. Your prefrontal cortex is that part of your brain responsible for high-level thinking, decision-making, and integrating information from your surroundings.
The prefrontal cortex connects to other brain regions that make neurochemicals like dopamine, oxytocin, and opioids, and in response to the placebo, these neurochemicals increase, causing even more opioid to be made by a brain region called the periaqueductal gray. Yes, your brain makes its own opioids naturally. Brain regions including anterior cingulate cortex, dorsolateral prefrontal cortex and basal ganglia have been activated following administration of placebo. Essentially, your brain orchestrates a whole symphony of activity when it expects healing to happen.
It Works Beyond Just Pain
Let’s talk scope here. Pain is the most studied area when it comes to placebo effects, but it’s far from the only one. Placebos have been shown to be most effective for conditions like pain management, stress-related insomnia, and cancer treatment side effects like fatigue and nausea. That’s a pretty impressive range already.
Research has highlighted a broad spectrum of conditions where placebo effects have demonstrated efficacy, including pain, Parkinson’s disease, depression, anxiety, addiction, with patients with depression experiencing nearly the same level of relief from a placebo as those treated with active medication. The fact that depression responds so strongly to placebos tells us something profound about the connection between expectation and mental health. It’s hard to say for sure, but this might completely change how we approach treatment in the future.
Fake Pills That Deliver Real Results
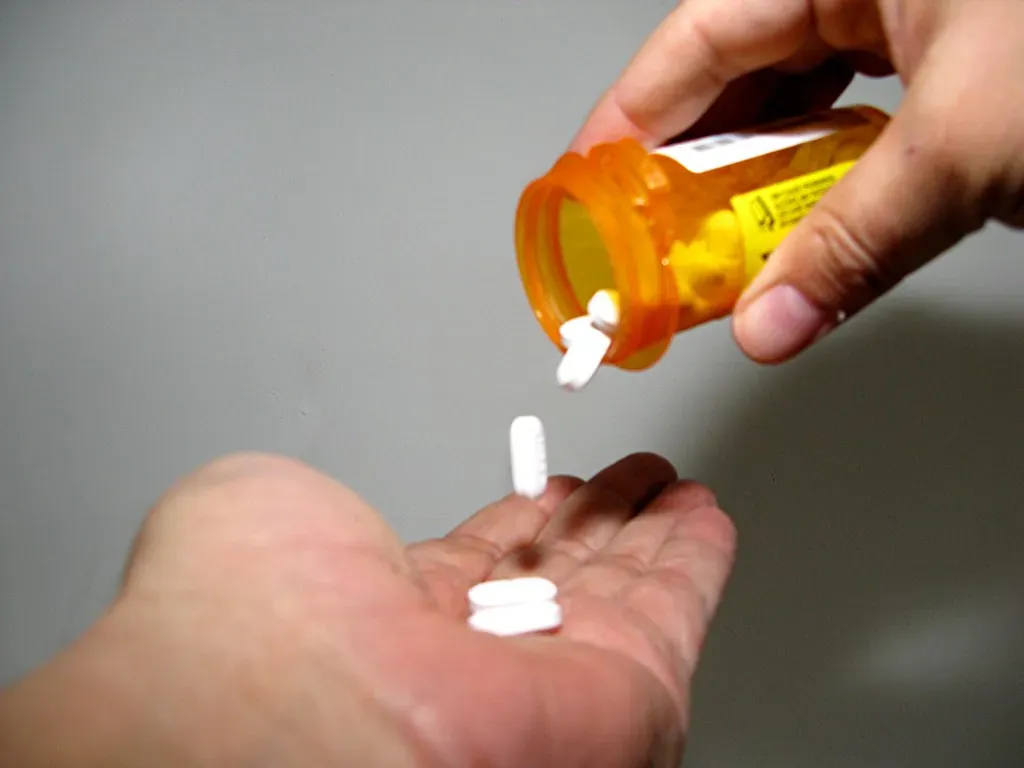
One of the wildest developments in placebo research is the concept of open-label placebos. Imagine being handed a pill and your doctor tells you straight up, “This is a sugar pill with no active ingredients.” Common sense would suggest it shouldn’t work, right? Surprisingly, it does. Patients with irritable bowel syndrome who received pills described truthfully as placebo pills made of an inert substance reported feeling better overall and having less severe symptoms than patients who received no treatment.
This isn’t an isolated finding. Emerging research shows that openly administered placebos can benefit patients with various medical conditions, and studies have analyzed effects of Open-Label Placebo on physical function and pain in individuals with chronic musculoskeletal pain. The implications are staggering. You don’t even need to be deceived for your brain to kickstart the healing process. Just the ritual of taking something, coupled with the context of treatment, can be enough.
Conditioning Your Brain to Heal

There’s another layer to this story, one that involves learning and memory. Your brain can be trained to associate certain cues with feeling better. Researchers taught mice to associate a distinctive environment with pain reduction by activating pain-suppressing neurons, and the animals then continued to experience pain relief in this environment even without neural stimulation. This shows conditioning at work.
People associate the ritual of taking medicine as a positive healing effect, and even if they know it’s not medicine, the action itself can stimulate the brain into thinking the body is being healed. Think about how many times you’ve felt a bit better just walking into a doctor’s office or taking that first sip of warm tea when you’re sick. Your brain picks up on those patterns and starts preparing your body for relief before the actual “medicine” even kicks in.
Not a Magic Cure for Everything

Let’s pump the brakes a bit here, because it’s important to be realistic. Placebos won’t lower your cholesterol or shrink a tumor, instead working on symptoms modulated by the brain like the perception of pain, and they may make you feel better but won’t cure you. This is crucial to understand. The placebo effect is powerful for subjective symptoms where the brain plays a big role in how you experience them.
You’re not going to cure cancer with positive thinking or treat diabetes with sugar pills. The lesson is about adding placebos to proven treatments and using them responsibly, understanding their incredible power to aid treatment of pain, depression and other maladies while recognizing their sizable limitations in curing life-threatening diseases. The goal is enhancement, not replacement.
How Doctors Already Use This Power

Here’s something that might surprise you. A 2013 study found that 97% of physicians acknowledged using some form of placebo during their career, which might be as simple as expressing strong belief in the likelihood that a patient will feel better from whatever treatment the doctor prescribes. Your doctor’s confidence in a treatment can actually influence how well it works for you.
The American Medical Association considers the placebo effect powerful enough that it’s ethical to use placebos to enhance healing on their own or with standard medical treatments if the patient agrees to it. This isn’t about trickery or abandoning real medicine. It’s about recognizing that the way treatment is delivered, the environment it’s given in, and the relationship between patient and doctor all contribute to outcomes. Smart clinicians are already tapping into this.
The Future of Harnessing Mind Power
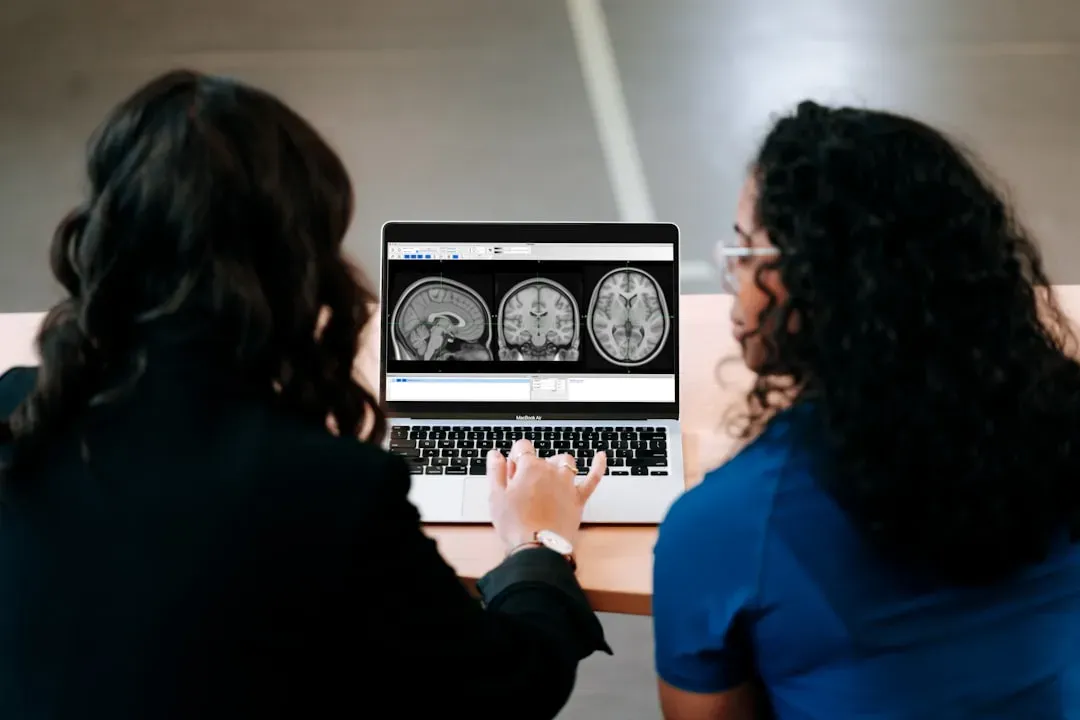
Scientists are working hard to understand exactly which people respond best to placebo effects and why. Researchers showed that they can reliably predict which chronic pain patients will respond to a sugar placebo pill based on the patients’ brain anatomy and psychological characteristics, as both personality and brain anatomy and functional properties are uniquely different between those responding to placebo and those not responding. Imagine getting a brain scan that tells you whether a placebo approach could help manage your chronic pain.
Those responding to a placebo have pain relief of about 30 percent, which is clinically significant and comparable or even superior to any drugs on the market. For some patients dealing with chronic pain, especially given the opioid crisis, being able to harness their brain’s natural pain-relief systems could be life-changing. The research is still evolving, but the potential here is enormous.
Conclusion

The placebo effect reveals something genuinely profound about who we are as human beings. Your mind isn’t separate from your body, it’s deeply intertwined with every physical process happening inside you. The fact that belief, expectation, and context can trigger real neurochemical changes, activate specific brain regions, and produce measurable healing effects should leave us all a bit awestruck. We’re walking around with this incredible capacity for self-healing, and we’re only just beginning to understand how to tap into it properly.
This doesn’t mean abandoning modern medicine or pretending that positive thoughts alone can cure serious diseases. Rather, it’s about recognizing that healing is a complex dance between physical treatments and mental states. The more we understand about this connection, the better we can design treatments that work with our brains instead of ignoring them. What do you think? Does it change your perspective knowing your brain has this much power over your body’s experience? Let us know in the comments.