If you wake up over 50 and feel like your body has a group chat you weren’t invited to, you’re not alone. Knees complain going downstairs, your back has opinions about chairs, and random twinges show up like uninvited guests. It can feel scary and confusing, and many people secretly wonder if these sensations mean something serious is wrong. In reality, for most otherwise healthy people, the story is a lot less dramatic and a lot more about normal biology and lifestyle than about illness.
That doesn’t mean you should ignore pain or “just accept it.” But it does mean many of these aches are your body sending status updates, not emergency alerts. Once you understand what’s really going on under the hood – how muscles, joints, nerves, hormones, sleep, and even your mood change with age – you can respond with smart, targeted changes instead of fear. Let’s unpack what might actually be behind those extra aches and what you can realistically do about them.
The Normal Wear-and-Repair Story: Your Body Is Not “Breaking,” It’s Adapting

One of the most surprising truths about midlife pain is that a lot of it comes from normal, expected changes in tissues that started decades ago. Your cartilage, tendons, and ligaments have been absorbing forces from walking, lifting, bending, and twisting since childhood. Over time, tiny microtears and structural changes accumulate. Your body is constantly trying to repair this, but the balance between wear and repair shifts a little with age. That does not mean your joints are crumbling; it means repair just takes longer, and the margin for error shrinks.
Think of your body like a favorite pair of high-quality jeans. After years of wear, the fabric softens, fades, and maybe thins in spots, but it’s still absolutely wearable and often more comfortable. Your tissues are similar: they bear a history of use. When you suddenly stand more, sit more, lift heavier, or stop moving for a while, those slightly “thinner” spots can start complaining. The key is not to assume the jeans are ruined, but to care for them differently – wash gentler, patch when needed, and stop pretending they’re brand new.
Muscle Loss and Stiffness: Why Skipping Strength Work Comes Back to Bite
Starting as early as your 30s and 40s, you naturally lose muscle mass and strength if you don’t actively work to maintain it. By the time you’re over 50, this quiet trend can really show up as more stiffness, fatigue, and soreness after activities that used to feel easy. Muscles act like shock absorbers for your joints; when they’re weaker or smaller, bones and cartilage take more of the hit. The result can be achier knees after a walk, a back that complains when you stand too long, or shoulders that grumble when you reach overhead.
The good news is that muscle is remarkably trainable, even in your 60s, 70s, and beyond. People of all ages can gain strength and reduce pain with simple, consistent resistance training: bodyweight squats, light dumbbells, resistance bands, or machines. I’ve seen plenty of people in their 50s say they thought their knee pain was “just getting old,” only to watch it dramatically improve after a few months of strength work. You’re not too old to lift; you’re too experienced not to.
Joint Changes and “Noisy” Knees: Degeneration Does Not Always Mean Disease

Imaging studies of people over 50 are almost shockingly consistent: a huge number show some degree of osteoarthritis, disc degeneration, bone spurs, or “wear-and-tear” changes, even in people without any pain. That means your X-ray results and your actual experience of pain don’t always match up. As cartilage thins a bit and joint surfaces become less perfectly smooth, you may feel more crunching, popping, or stiffness, especially first thing in the morning or after sitting still. These sensations are often unnerving but not automatically dangerous.
The real issue is how these structural changes interact with your daily habits. Long stretches of sitting, sudden bursts of heavy activity after a sedentary week, or carrying extra body weight can all increase the load on joints that are already a bit less forgiving. Instead of viewing this as “my joints are ruined,” it’s more accurate to see it as “my joints need a smarter operating plan.” Regular low-impact movement, strength training around the joint, and weight management can dramatically ease discomfort, even if the pictures of your joints never look “perfect” again.
Nerves, Pain Sensitivity, and the Brain’s “Alarm System” Aging
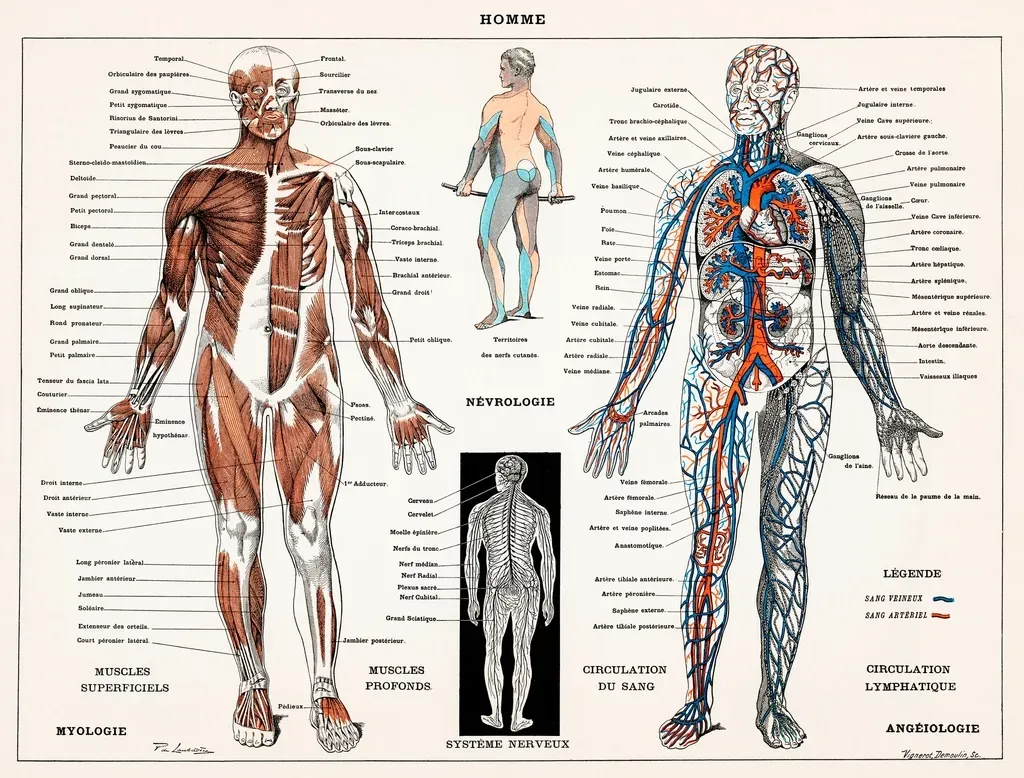
Pain is not just about tissues; it’s about how your nervous system interprets signals. As we age, the way the brain and nerves process information can change. A minor irritation that your brain once ignored may now set off a louder alarm. Sleep issues, stress, and past injuries can turn up the volume even more. The result is that your aches can feel more intense or more persistent, even if the underlying physical change is not severe.
Think of your nervous system as a home security system that has slowly been made more sensitive over the years. At first, it only reacted to a real break-in; now it may go off if a branch brushes the window. That does not mean you are imagining your pain, and it does not mean you are sick. It means your system is on high alert. Calming that system – through better sleep, stress management, graded exercise, and activities that relax the nervous system like walking in nature or gentle stretching – can dial down pain even when scans do not “fix” anything.
Hormones, Inflammation, and the Midlife “Background Noise”
For many people, especially women, the years around 50 come with big hormonal shifts. Changes in estrogen and other hormones can affect how joints feel, how muscles recover, and how sensitive you are to discomfort. At the same time, there tends to be a slow rise in low-level background inflammation linked to things like chronic stress, poor sleep, excess belly fat, and inactivity. You might not have an inflammatory disease, but your whole system can feel a bit more irritated and reactive.
This background noise shows up as vague stiffness, aching after normal activity, or feeling “old” when you first get moving. The empowering part is that daily lifestyle choices can have a surprisingly big impact here. Eating more whole, minimally processed foods, prioritizing sleep, managing stress with real tools rather than just powering through, and building a movement routine can all turn down that inflammatory hum. You may not be able to control every hormone shift, but you have more influence over your discomfort than it often feels like in the moment.
Sitting, Screens, and “Modern Life Body”: It’s Not Age, It’s Habit

Blaming age is easy; blaming the seven hours hunched over a laptop or scrolling on the couch is harder, but often more honest. A lot of what we call “aging pain” is really “repetitive position pain.” Your body adapts fiercely to what you do most. If that is sitting, you will get very good at sitting and not so great at everything else. Hips tighten, chest muscles shorten, upper back and glute muscles weaken, and then anything outside that narrow pattern – walking fast, lifting a suitcase, climbing stairs – feels uncomfortable.
I catch myself in this trap too: a long writing day, then suddenly my neck and lower back ache and my first instinct is to wonder what is “wrong” with me. Most of the time, what is wrong is that my body wasn’t meant to be parked in one position for half the day. Small, consistent changes – standing up every half hour, walking calls, stretching breaks, varying your work setup – can drastically change how achy you feel. You do not need a perfect ergonomic setup to feel better; you need less stillness and more variety.
Sleep, Stress, and Mood: Why Everything Hurts More When Life Is Heavy

If you have ever noticed that everything hurts more after a terrible night of sleep or a stressful week, that is not your imagination. Poor sleep lowers your pain threshold, messes with hormone balance, and impairs tissue repair. Stress floods your body with chemicals that are incredibly useful in short bursts but exhausting and inflammatory when they never let up. Over 50, you may be juggling aging parents, adult children, financial worries, and health concerns – your body carries all of that.
Depression and anxiety can also amplify physical pain, and the relationship goes both ways. Feeling achy makes you move less and withdraw, which then worsens mood, which then worsens pain. This is not about your aches being “all in your head.” It is about recognizing that pain is a full-body experience that includes the brain and emotions. Protecting your sleep like it is a prescription, building in stress relief that actually works for you, and, when needed, getting support for mental health are not luxuries. They are direct, evidence-based ways to reduce physical pain.
When to Worry: Red Flags Versus Normal Aging Signals
None of this means you should dismiss every ache as “just getting older.” Some symptoms do deserve urgent attention. Sudden, severe pain that comes out of nowhere, pain with significant swelling or deformity, unexplained weight loss, pain with fever or night sweats, chest pain, or pain that wakes you every single night and is not position-dependent – these are not typical “I sat too long” signals. In those situations, getting checked by a healthcare professional promptly is wise, not dramatic.
The flip side is that many everyday pains do not fit that red-flag profile and are more like feedback from your body than cries for help. A knee that aches after a long walk but settles with rest and gentle movement, a stiff back that improves through the day, or shoulders that feel better as you get stronger usually point to mechanical and lifestyle factors, not hidden disease. Learning to distinguish between “this needs evaluation” and “this needs smarter care” is one of the most powerful skills you can build in your 50s and beyond.
What You Can Actually Do: Building a Body That Hurts Less in Your 50s and Beyond

The most encouraging takeaway is that normal aging does not doom you to a life of constant pain. There is strong evidence that a few unglamorous habits make a huge difference: regular strength training two or three times a week, daily walking or other low-impact cardio, and frequent movement snacks to break up sitting. Add to that decent sleep, mostly whole-food eating, and real stress management, and you have a simple but powerful toolkit. None of it is revolutionary, but the impact over a few months can feel pretty close to magic.
In practice, that might look like this: a 20-minute home routine with bodyweight squats, wall push-ups, and hip bridges; a daily walk after dinner; stretching hips and chest during TV time; setting a timer to stand every half hour at work; going to bed a bit earlier most nights. You do not have to be perfect or turn into an athlete. You just have to be consistently slightly kinder to your future self. Over time, your body starts to feel less like a problem and more like a teammate again.
Conclusion: You’re Not Broken – You’re Being Asked to Evolve

It is easy, over 50, to interpret every new ache as evidence that you are falling apart or secretly sick. The more honest and hopeful interpretation is that your body is changing and demanding better support. Muscle, joints, nerves, hormones, sleep, and mood all shift with time, and many of the pains you feel are the natural consequences of those shifts colliding with modern, sedentary, high-stress living. That is not a personal failure or a medical crisis; it is a wake-up call.
My own opinion, after watching a lot of people navigate this stage, is that blaming “old age” is one of the most damaging habits we pick up. It lets us off the hook and quietly steals our options. You are not fragile glass; you are more like a seasoned tree that may creak in the wind but has deep, powerful roots. If you treat every ache as a cue to move smarter, sleep better, lift something, and care more, your 50s and beyond can be less about decline and more about renegotiation. If your body could talk, what small change would it ask for first?



